| Journal of Clinical Gynecology and Obstetrics, ISSN 1927-1271 print, 1927-128X online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Clin Gynecol Obstet and Elmer Press Inc |
| Journal website https://jcgo.elmerpub.com |
Original Article
Volume 000, Number 000, March 2025, pages 000-000
Novel Multimodal Radiofrequency Therapy for Mixed Urinary Incontinence: A Pilot Study
Pablo Gonzalez Isazaa , Diana Lorena Velez Rizob, c
aUrogynecology and Reconstructive Pelvic Surgery Unit, Obstetrics and Gynecology Department, Hospital Universitario San Jorge, Pereira, Colombia
bDepartment of Women Health, Fundacion Cardioinfantil La Cardio, Bogota, Colombia
cCorresponding Author: Diana Lorena Velez Rizo, Fundacion Cardioinfantil La Cardio, Bogota, Colombia
Manuscript submitted December 21, 2024, accepted March 17, 2025, published online March 28, 2025
Short title: Multimodal Radiofrequency Therapy for MUI
doi: https://doi.org/10.14740/jcgo1501
| Abstract | ▴Top |
Background: Mixed urinary incontinence (MUI) significantly affects patients’ quality of life (QOL) and poses a therapeutic challenge owing to its multifactorial etiology. Traditional treatments, including pharmacotherapy and surgery, often yield suboptimal outcomes or entail considerable risk. This study aimed to evaluate the efficacy and safety of a novel multimodal radiofrequency (MMRF) therapy for improving MUI symptoms, QOL and histological markers of pelvic tissue integrity.
Methods: A prospective pilot study was conducted on 20 female patients diagnosed with MUI. Participants underwent MMRF therapy, which consisted of two modalities: Morpheus V, delivering fractional radiofrequency energy, and Forma V, providing bipolar energy for superficial tissue tightening (Empower Bipolar Radiofrequency Platform InMode Aesthetics, Lake Forest, California, Serial Number R30326211). Treatment was administered over two to three sessions with follow-up at 3 and 6 months. Subjective outcomes were assessed using validated scales, including the International Consultation on Incontinence Questionnaire-Short Form (ICQ-SF), Potenziani scale, overactive bladder symptom score (OAB-SS), and QOL measures using a visual analog scale (0 - 10). Punch biopsies from the anterior vaginal wall were obtained at baseline and at 6 months to evaluate histological changes. Statistical analyses were performed to determine the significance of the pretreatment and posttreatment differences.
Results: Twenty participants were included in this study. ICQ-SF scores decreased from 14.05 ± 4.22 at baseline to 10.05 ± 3.79 at 3 months and 7.65 ± 4.44 at 6 months (P < 0.01). The Potenziani and OAB-SS scores exhibited similar reductions, indicating enhanced bladder control and urgency relief (P < 0.001). QOL improved significantly, with mean QOL scores declining from 6.00 ± 1.03 at baseline to 2.95 ± 0.94 at 6 months (P < 0.001). Histological analyses revealed increased collagen density, enhanced vascularization, and reduced inflammatory infiltrates, supporting tissue remodeling and functional recovery.
Conclusions: MMRF therapy is a safe, effective and minimally invasive treatment for MUI that addresses both the structural and functional contributors to incontinence. Significant improvements in symptom severity, QOL, and tissue integrity position of MMRF are promising non-surgical options for managing pelvic floor dysfunction. Further research with larger populations and extended follow-up is recommended to confirm these findings and to establish MMRF as a standard treatment for MUI.
Keywords: Mixed urinary incontinence; Quality of life; Multimodal radiofrequency; Safety
| Introduction | ▴Top |
Mixed urinary incontinence (MUI) is a prevalent condition, especially among women, and is characterized by a combination of stress and urgency urinary incontinence. Affecting the quality of life (QOL), MUI imposes a considerable psychological and social burden on up to 15.7-20.5% of women in the United States in the 2017 - 2018 cycle. This prevalence was higher in women aged 60 years and older (12.9-19.0%) [1], with similar values in other locations [2] and a mean annual worldwide incidence of all-types urinary incontinence ranging from 1% to 9% [3]. Traditional management approaches include lifestyle modifications, pharmacological therapy, pelvic floor exercises, and surgical interventions for severe cases [4-8]. Despite these options, many patients experience limited efficacy, side effects or poor long-term adherence to treatment regimens [9-11]. In recent years, energy-based devices have emerged as minimally invasive alternatives that utilize lasers, radiofrequency (RF), and high-intensity focused ultrasound technologies. These modalities promote collagen remodeling and tissue tightening, potentially improving the structural and functional integrity of the pelvic floor and urethral support. Among these, multimodal radiofrequency (MMRF) technologies, including Morpheus V and Forma V, have shown promise in enhancing vaginal and urethral tissue health [7, 12, 13]. However, robust evidence of their efficacy in managing MUI remains sparse, necessitating further research [14, 15].
While emerging technologies have gained traction, critical gaps persist in understanding their long-term efficacy and mechanisms of action in MUI. Previous studies have primarily focused on subjective symptom improvement, often relying on patient-reported outcomes without correlating them with objective biomarkers or histological data [16, 17]. Furthermore, research often emphasizes single modalities or fails to account for the multifaceted nature of MUI, which encompasses both structural and functional deficiencies [18-20]. The clinical applicability of MMRF therapy, which combines tissue remodeling and neuromodulation effects, has yet to be thoroughly evaluated. This evaluation requires comprehensive studies integrating patient-reported outcome measures (PROMs) and objective outcome measures [9] to delineate the true potential of these technologies for MUI management.
We hypothesized that MMRF therapy using Morpheus V and Forma V could significantly improve MUI symptoms by enhancing the structural support and neuromuscular function of the pelvic floor. This hypothesis is grounded in the dual action of RF technology, which promotes tissue tightening and modulates the overactive bladder pathways. The central research question is whether this therapy leads to measurable improvements in validated outcome scores, including the International Consultation on Incontinence Questionnaire-Short Form (ICIQ-SF), Potenziani scale, and overactive bladder symptom score (OAB-SS) while correlating these outcomes with the histological changes observed through punch biopsies. This study aimed to provide a comprehensive evaluation of MMRF technology as a novel, minimally invasive treatment for MUI, bridging the gap between subjective symptom relief and objective tissue-level outcome changes.
To address these gaps, we employed a systematic approach involving a 6-month follow-up of patients undergoing Morpheus V and Forma V therapies. This study integrated PROMs and objective evaluation methods, including validated questionnaires and punch biopsies, to provide a holistic assessment of therapy outcomes. By combining two complementary RF modalities, our approach sought to leverage the synergistic effects of deep tissue remodeling and surface-level tightening, targeting both structural and functional contributors to MUI. This dual-action mechanism represents a novel paradigm for non-surgical MUI treatment. Importantly, this study fills critical gaps in the current literature by linking patient-reported outcomes to histological changes, thereby providing new insights into the mechanisms underlying symptom improvement. Our findings aim to guide clinical decision-making and establish MMRF therapy as a viable evidence-based option for managing MUI.
| Materials and Methods | ▴Top |
Study design and setting
A prospective, descriptive, experimental pilot study was conducted between August 2023 and February 2024 at the Urogynecology Unit of the Obstetrics and Gynecology Department at the Hospital Universitario San Jorge in Pereira, Colombia.
Participants
Adult female patients presenting with clinically diagnosed MUI, a condition defined by concurrent symptoms of stress and urgency urinary incontinence, were invited to participate. To ensure homogeneity and reliability, strict inclusion and exclusion criteria were used. Women with no prior pelvic organ prolapse (POP) surgeries and willingness to adhere to a 6-month follow-up protocol were eligible. Conversely, patients with advanced POP (pelvic organ prolapse quantification (POP-Q) stage > 1), undiagnosed uterine bleeding, or a history of rectovaginal or vesicovaginal fistulas were not considered. Additional exclusion criteria were current smokers, individuals undergoing concurrent energy-based therapies or pelvic floor rehabilitation, and those with significant medical comorbidities that could confound the study results. These criteria were carefully chosen to focus on a population that would benefit the most from MMRF therapy and to eliminate factors that might influence the outcomes.
MMRF therapy
MMRF therapy was delivered using a two-step protocol combining Morpheus V and Forma V technologies (Fig. 1). The first step involved the Morpheus V probe, which features a transparent casing with visible internal circuitry and utilizes fractional RF energy delivered at 1 MHz and peak power of 65 W. A specialized probe equipped with 24 microneedles was used to target specific areas within the vaginal cavity, particularly those contributing to continence mechanisms. The microneedles allowed for adjustable penetration depths of 1 - 3 mm, delivering approximately 200 mJ per pulse to remodel the tissue through thermal energy while minimizing damage to the surface layers. The temperature used during the two steps of RF therapy depends on the device used. Morpheus8 V delivered fractional bipolar RF at temperatures of 58 °C and 61 °C, and Forma V delivered bipolar RF at 40 °C and 43 °C. The second step employed the Forma V probe equipped with flat and spherical electrodes that delivered 1 MHz with a peak power of 40 W through a bipolar RF modality. This phase aims to provide surface-level tissue tightening and neuromodulation through rectangular pulse configurations using a specially designed ergonomic probe. Both modalities have integrated cooling systems and built-in impedance sensors and were administered in multiple sessions at predetermined intervals as part of a structured rehabilitation program. The duration of the sessions depended on the patient and was not standard. Morpheus8 V session time depended on the number of passes (usually three passes with different levels of energy and depth of penetration were performed), and the Forma V bipolar RF lasted 20 min. The interval between sessions depended on the device used. Morpheus8 V consisted of three sessions at 4-week intervals, and Forma V consisted of six sessions at 2-week intervals. All procedures were performed under standardized conditions by trained and experienced nurses from the study center.
 Click for large image | Figure 1. Morpheus V (left) and Forma V (right) probes. |
Outcome measures
Both PROMs and objective outcome measures were incorporated to evaluate the efficacy of MMRF therapy comprehensively. PROMs included validated scales such as the ICIQ-SF [21, 22], Potenziani scale (Potenziani-14-CI-IO-QOL-2000) [23], and OAB-SS [24], all of which were administered at baseline and 6 months post treatment. These instruments provided quantitative assessments of symptom severity, patient QOL, and functional impact of MUI [25]. For objective evaluation, punch biopsies were collected from the anterior vaginal wall at the urethrovaginal junction before therapy initiation and after 6 months. Histological analysis (hematoxylin/eosin) of these samples aimed to identify morphological and structural changes indicative of therapeutic effects, including collagen remodeling and vascular alterations. Integrating PROMs and objective measures was intended to provide a comprehensive understanding of the treatment efficacy.
Ethical considerations
The study adhered to the ethical principles outlined in the international guidelines, including the Declaration of Helsinki, Belmont Report, and Council for International Organizations of Medical Sciences (CIOMS) standards. All participants provided written informed consent after receiving detailed explanations of the study’s purpose, procedures, risks, and benefits. This research was classified as minimal-to-beyond-minimal risk, as supported by preclinical and clinical evidence demonstrating the safety of RF-based interventions in humans. Ethical approval was obtained from the hospital’s ethics committee to ensure compliance with national regulations. Measures to protect the participants included anonymized data collection, secure storage of medical records, and the option to withdraw at any time without consequences.
Statistical analysis
Continuous variables were reported as means with standard deviations (SD), whereas categorical variables were analyzed using the Chi-square test. Pretreatment and posttreatment scores on validated scales were compared using Mann-Whitney, Kruskal-Wallis, and Dunn pairwise tests to determine the significance of the observed changes. Histological findings from punch biopsies were evaluated qualitatively and quantitatively to assess tissue-level changes according to clinical outcomes. Statistical significance was set at P < 0.05.
| Results | ▴Top |
Participant characteristics
Twenty participants were included in the study, with a mean age of 56.15 years (SD 9.78), ranging from 44 to 84 years. The median parity among the participants was three, with the majority (40%) having three live births. Approximately 60% of the participants presented with POP-Q stage 0, and the remaining 40% presented with stage 1. Most participants (65%) completed three treatment sessions, whereas the remainder underwent two sessions. Baseline urodynamic evaluations revealed a mix of normal findings and variable abdominal leak point pressures (ALPPs) distributed across the different thresholds (Table 1). None of the 20 patients presented adverse events, unwanted treatment-related symptoms, or complications.
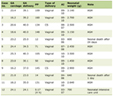 Click to view | Table 1. Baseline Clinical Characteristics |
PROMs
The mean baseline score for the ICQ-SF was 14.05 (SD 4.22), reflecting moderate symptom severity. At 3 months, the mean score reduced to 10.05 (SD 3.79), with a further decrease to 7.65 (SD 4.44) by 6 months. Significant improvements in ICQ-SF scores at both 3 and 6 months compared with baseline were observed (P < 0.01). Similarly, the Potenziani scores demonstrated marked improvement over time. The baseline scores averaged 12.55 (SD 2.44), decreasing to 10.05 (SD 2.06) at 3 months and 6.20 (SD 1.91) at 6 months. The changes were statistically significant, with a robust correlation observed between the baseline and follow-up scores (Pearson’s correlation, r = 0.89, P < 0.001).
The mean OAB-SS at 3 months was 11.68 (SD 2.45), decreasing to 8.68 (SD 1.45) at 6 months, representing an improvement of 25.7%. A statistically significant reduction in OAB-SS scores was observed between these time points (P < 0.01), with a moderate correlation (r = 0.64). QOL measures demonstrated substantial improvement, aligning with the reductions in symptom severity. Scores averaged 6.00 (SD 1.03) at 3 months and declined to 2.95 (SD 0.94) at 6 months (P < 0.001). These improvements reflected enhanced posttreatment patient satisfaction and perceived well-being (Table 2).
 Click to view | Table 2. PROMs Mean (SD) Score and Percentage of Improvement |
Histological findings
Punch biopsies taken from the anterior vaginal wall revealed notable posttreatment tissue remodeling. Collagen density increased at 6 months compared with baseline, with evidence of enhanced vascularization, epithelial maturation, and reduced inflammatory infiltrates. These histological changes corroborated the observed clinical improvements, suggesting that MMRF therapy effectively promotes tissue regeneration and functional restoration (Figs. 2, 3).
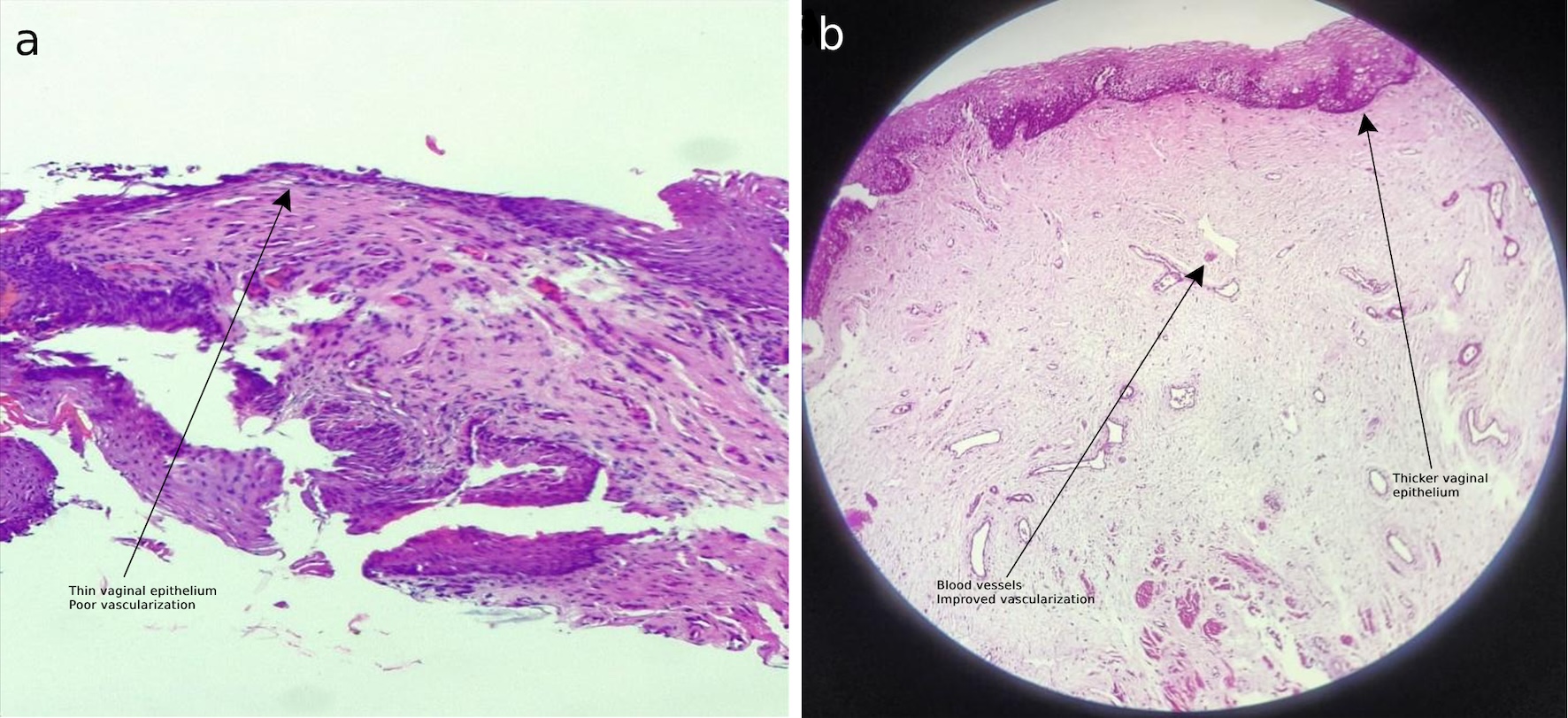 Click for large image | Figure 2. Histological findings. (a) Before protocol: atrophic epithelium. (b) Poor epithelial maturation. |
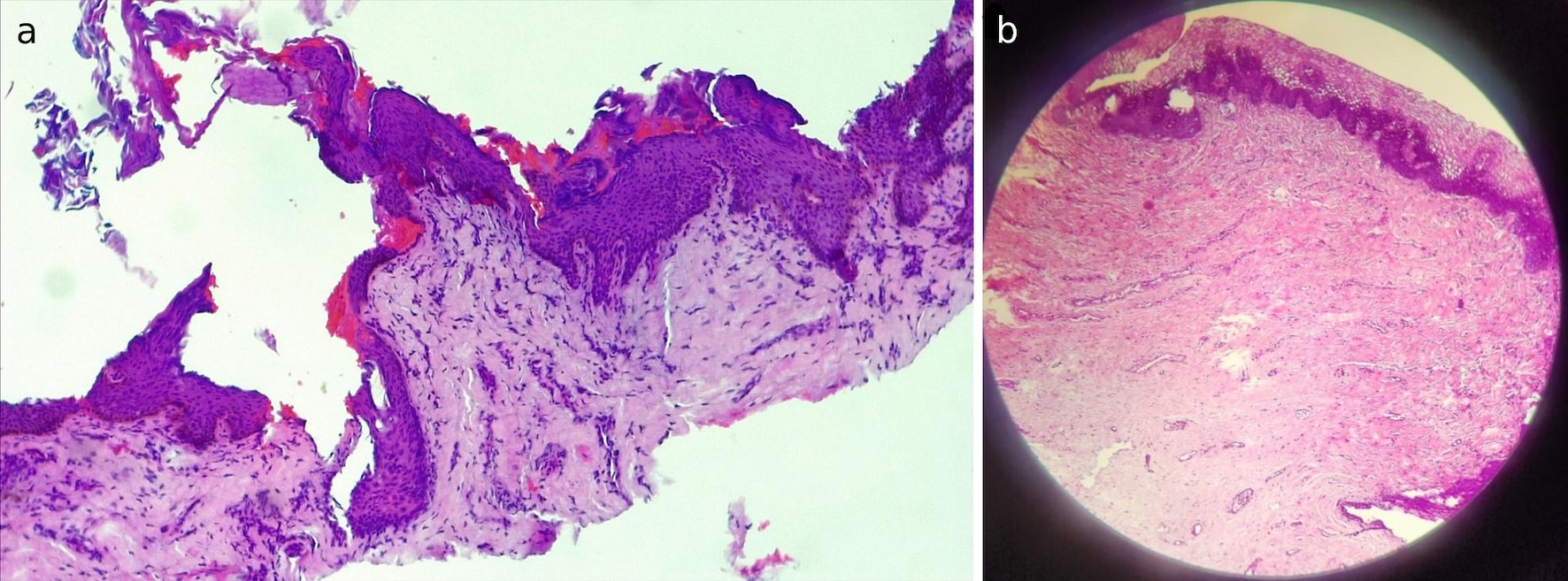 Click for large image | Figure 3. Histological findings. (a) 6 months after the treatment protocol: increased epithelium maturation and vascularity. (b) Increased epithelial maturation, dense stroma papillae formation, and increased vascularization. |
Correlation analysis
Significant correlations were found between the baseline and follow-up scores for all scales, indicating the consistency of improvements. Potenziani scores showed the strongest correlation (r = 0.89, P < 0.001), followed by ICQ-SF (r = 0.54, P < 0.01) and OAB-SS (r = 0.64, P < 0.01).
| Discussion | ▴Top |
We found that MMRF was both effective and safe. Over 6 months, it produced significant improvements in validated scales, such as the ICQ-SF, Potenziani scale and OAB-SS. Furthermore, the improvement in QOL underscores the meaningful impact of therapy on daily living. Histological analyses provided complementary evidence, revealing increased collagen density and enhanced vascularization in treated tissues. These results on a novel treatment approach support the hypothesis that MMRF acts through mechanisms distinct from conventional pharmacotherapy, offering a promising alternative for patients who are either non-responders or intolerant to traditional treatments.
Our findings align with those of recent studies on energy-based modalities, including RF [12, 15, 17-20, 26], which corroborate this mechanism, emphasizing the role of thermal energy in collagen contraction and neocollagenesis. In 2013, Chinthakanan et al conducted a randomized controlled trial comparing low-energy RF vaginal therapy to sham treatment in postmenopausal women with mild to moderate stress urinary incontinence (SUI). Among the 49 participants, the RF group (n = 23) achieved a 69.6% success rate at 1 year, defined by improvements in the 1 h pad weight test, compared to 38.5% in the sham group. However, secondary outcomes, such as the incontinence quality of life (I-QOL) and urogenital distress inventory-6 (UDI-6) were not statistically different [20]. On the other hand, in 2024, Rabiai et al investigated the addition of monopolar non-ablative RF to pelvic floor muscle training (PFMT) in a randomized controlled trial of 38 women with moderate SUI. The RF group (n = 18) achieved a 9.4-point reduction in ICIQ-SF scores (95% confidence interval (CI): -12.6 to -6.3), surpassing the minimal clinically important difference, compared to a 3.9-point reduction (95% CI: -6.9 to 1.0) in the PFMT-only group. Additionally, the experimental group exhibited significant improvements in the 1 h pad test (P < 0.05) and fewer weekly SUI episodes, with a time-group interaction effect observed over 6 months (P < 0.001) [18].
In 2024, Long et al evaluated the Viveve® System, applying 90 J/cm2 of fractional RF energy in a single session to 34 women with SUI. At 6 months, significant reductions in SUI symptoms were reported, with improved scores in the UDI-6 (-3.1 points), Incontinence Impact Questionnaire-7 (-2.8 points) and ICIQ-SF (-4.5 points), along with reduced bladder neck mobility and proximal urethral rotation angle. Sexual function also improved, as evidenced by increased Female Sexual Function Index scores in all domains except for pain [15]. In 2023, Abdelaziz et al explored the safety and short-term efficacy of fractional bipolar RF delivered through microneedling in 20 women with MUI and genitourinary syndrome of menopause (GSM). Using the EmpowerRF platform, significant symptom improvements were observed at 1, 3, and 6 months post treatment. For example, UDI-6 scores decreased from 37.2 to 25.4, and I-QOL scores improved by 45%. Histological findings revealed enhanced collagen remodeling and neocollagenesis, providing a mechanistic basis for the observed benefits [19]. Furthermore, the neuromodulatory effects of RF energy, which may influence bladder hyperactivity and urgency symptoms, offer an additional explanation for improvements in urgency-related scales [26, 27]. This dual-action mechanism, which combines structural reinforcement with functional modulation, underscores the unique therapeutic potential of MMRF for MUI.
Although promising, this study has limitations. The small sample (n = 20) limits generalizability, and the single-center design without a control group introduces potential biases. The 6-month follow-up, while sufficient for initial efficacy, does not assess long-term outcomes. The absence of baseline data further limits evaluation. The lower OAB-SS improvement between 3 and 6 months may reflect a ceiling effect or reduced sensitivity to change, as indicated by score clustering at 3 months. In contrast, broader measures like QOL and Potenziani scales continued detecting improvements. Despite these limitations, rigorous methodologies and validated measures enhance result reliability [21, 22, 24] and ensure that the observed improvements are both clinically meaningful and statistically robust. Moreover, the consistent alignment between subjective reports and objective histological findings strengthens our conclusions. The absence of adverse events further supports the feasibility and safety of MMRF therapy, making it a viable alternative for patients seeking noninvasive options. Anticipated criticisms regarding the sample size or lack of controls are mitigated by the pilot nature of this investigation, which serves as a necessary foundation for future large-scale studies.
The findings from this pilot study pave the way for future research to build upon these insights. Larger, multicenter, randomized controlled trials are essential to validate the efficacy and safety of MMRF therapy. These studies should aim to compare MMRF with established treatments such as pharmacotherapy, pelvic floor physical therapy and surgical interventions to determine their relative effectiveness and cost efficiency. Extended follow-up periods are also necessary to evaluate the durability of symptom relief and the progression of histological changes over time. Additionally, mechanistic studies exploring the neuromodulatory effects of RF energy could provide deeper insights into the pathways involved, potentially identifying biomarkers for predicting treatment responses and optimizing patient selection.
The MUI is a multifaceted condition that profoundly impacts patients’ physical and psychological well-being. Current treatment options often fail to address both the structural and functional contributors to incontinence, leaving a significant proportion of patients dissatisfied or untreated. This study positions MMRF therapy as a transformative approach that bridges the gap between conservative and surgical treatment. By simultaneously targeting tissue integrity and bladder function, the MMRF offers a comprehensive solution that is minimally invasive, safe and effective. Its ability to improve the QOL while avoiding the risks and recovery times associated with surgery makes it a particularly attractive option in the continuum of care for pelvic floor dysfunction.
Conclusion
Our study demonstrates that MMRF is a promising noninvasive treatment for MUI. MMRF addresses critical gaps in the current therapeutic landscape by significantly reducing symptom severity, improving QOL, and promoting histological tissue remodeling. Although further research is needed to confirm these findings in larger and more diverse populations, the results of this pilot study highlight the MMRF as an innovative and effective option for managing MUI. This approach offers hope for patients seeking relief from a condition that has long been challenging to treat, marking an important step forward in pelvic floor health.
Acknowledgments
We would like to express our sincere gratitude to the patients who participated in this study and to the dedicated team at the Urogynecology Unit of the Hospital Universitario San Jorge for their unwavering support throughout this research. Special thanks are also extended to the nursing staff for their expertise in administering MMRF and assisting with patient follow-up.
Financial Disclosure
This study was conducted without external funding. The authors declare that no financial support has been received for the research, authorship or publication of this article.
Conflict of Interest
The authors declare no conflicts of interest regarding the publication of this paper.
Informed Consent
All participants provided written informed consent.
Author Contributions
PGI was responsible for the conception, design and first draft of the manuscript, as well as data collection and analysis. DLVR contributed to the interpretation of data, critically revised the manuscript for important intellectual content and provided the final approval of the version to be published.
Data Availability
The data supporting the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
ALPP: abdominal leak-point pressures; I-QOL: incontinence quality of life; ICQ-SF: International Consultation on Incontinence Questionnaire-Short Form; MUI: mixed urinary incontinence; MMRF: multimodal radiofrequency; OAB-SS: overactive bladder symptom score; PROMs: patient-reported outcome measures; PFMT: pelvic floor muscle training; POP: pelvic organ prolapse; QOL: quality of life; UDI-6: urogenital distress inventory
| References | ▴Top |
- Abufaraj M, Xu T, Cao C, et al. Prevalence and trends in urinary incontinence among women in the United States, 2005-2018. Am J Obstet Gynecol. 2021;225:166.e1-166.e12.
doi - Osama M, Shaukat S, Javed M, Naeem M. Prevalence of urinary incontinence among young female adults. J Pak Med Assoc. 2022;72(11):2283-2287.
doi pubmed - Milsom I, Gyhagen M. The prevalence of urinary incontinence. Climacteric. 2019;22(3):217-222.
doi pubmed - Balk EM, Rofeberg VN, Adam GP, Kimmel HJ, Trikalinos TA, Jeppson PC. Pharmacologic and nonpharmacologic treatments for urinary incontinence in women: a systematic review and network meta-analysis of clinical outcomes. Ann Intern Med. 2019;170(7):465-479.
doi pubmed - Game X, Dmochowski R, Robinson D. Mixed urinary incontinence: Are there effective treatments? Neurourol Urodyn. 2023;42(2):401-408.
doi pubmed - Painter CE, Suskind AM. Advances in pharmacotherapy for the treatment of overactive bladder. Curr Bladder Dysfunct Rep. 2019;14(4):377-384.
doi pubmed - Costa A, Vasconcellos IM, Pacheco RL, Bella Z, Riera R. What do Cochrane systematic reviews say about non-surgical interventions for urinary incontinence in women? Sao Paulo Med J. 2018;136(1):73-83.
doi pubmed - NICE Guidance - Urinary incontinence and pelvic organ prolapse in women: management: (c) NICE (2019) Urinary incontinence and pelvic organ prolapse in women: management. BJU Int. 2019;123(5):777-803.
doi pubmed - Shah GS, Phillips C. What women want now! Eur J Obstet Gynecol Reprod Biol. 2023;286:118-120.
doi pubmed - Jha S, Jeppson PC, Dokmeci F, Marquini GV, Sartori MGF, Moalli P, Malik SA. Management of mixed urinary incontinence: IUGA committee opinion. Int Urogynecol J. 2024;35(2):291-301.
doi pubmed - Qatawneh A, Lari FN, Sawas WA, Alsabree FA, Alowaisheer MK, Aldarawsheh MA, Alshareef RA. Management of stress urinary incontinence by obstetricians and gynecologists in jordan: a nationwide survey study. Healthcare (Basel). 2024;12(15):1489.
doi pubmed - Vanaman Wilson MJ, Bolton J, Jones IT, Wu DC, Calame A, Goldman MP. Histologic and clinical changes in vulvovaginal tissue after treatment with a transcutaneous temperature-controlled radiofrequency device. Dermatol Surg. 2018;44(5):705-713.
doi pubmed - Karcher C, Sadick N. Vaginal rejuvenation using energy-based devices. Int J Womens Dermatol. 2016;2(3):85-88.
doi pubmed - Millheiser LS, Pauls RN, Herbst SJ, Chen BH. Radiofrequency treatment of vaginal laxity after vaginal delivery: nonsurgical vaginal tightening. J Sex Med. 2010;7(9):3088-3095.
doi pubmed - Long CY, Chang CY, Sung IC, Loo ZX, Lin KL. The therapeutic effect of monopolar radiofrequency therapy on urinary symptoms and sexual function. Biomedicines. 2024;12(10):2288.
doi pubmed - Rothenberger R, Kopinga E, Dell J, Moore RD, Miklos JR, Karram M. Use of radiofrequency ablation of the vaginal canal for genitourinary syndrome of menopause. J Sex Med. 2025;22(1):51-56.
doi pubmed - Pereira GMV, Almeida CM, Martinho N, de Andrade KC, Juliato CRT, Brito LGO. Pelvic floor muscle training vs radiofrequency for women with vaginal laxity: randomized clinical trial. J Sex Med. 2024;21(8):700-708.
doi pubmed - Er-Rabiai Y, Torres-Lacomba M, Casana J, Lopez-Bueno R, Nunez-Cortes R, Calatayud J. The effectiveness of adding transvaginal radiofrequency to pelvic floor muscle training for 6 weeks in women with stress urinary incontinence. a double-blind randomised controlled trial. Int Urogynecol J. 2024;35(9):1817-1828.
doi pubmed - Abdelaziz A, Blusewicz TA, Coley KP, Karram M. Safety, tolerability and short-term efficacy of transvaginal fractional bipolar radiofrequency therapy for symptoms of stress and or mixed incontinence in conjunction with genitourinary syndrome of menopause. Neurourol Urodyn. 2023;42(4):807-813.
doi pubmed - Chinthakanan O, Saraluck A, Kijmanawat A, Aimjirakul K, Wattanayingcharoenchai R, Manonai J. Comparison of low-energy radiofrequency thermal vaginal therapy with sham treatment for stress urinary incontinence in postmenopausal women: a randomized controlled trial. Int J Womens Health. 2023;15:1779-1790.
doi pubmed - Patino ID Validacion del ICIQ-UI SF en una poblacion de Bogota, y su relacion con el tipo y severidad de la incontinencia. Estudio prospectivo metacentrico.
- Espuna Pons M, Rebollo Alvarez P, Puig Clota M. [Validation of the Spanish version of the International Consultation on Incontinence Questionnaire-Short Form. A questionnaire for assessing the urinary incontinence]. Med Clin (Barc). 2004;122(8):288-292.
doi pubmed - Potenziani Cuestionario de impacto de la incontinencia urinaria en la calidad de vida de la mujer (Potenziani-14-CI-IO-QOL2000). Asociacion Espanola de Urologia.
- Espuna Pons M, Puig Clota M, Rebollo Alvarez P. [Validation of the Spanish version of the "Bladder control Self-Assessment Questionnarie" (B-SAQ). A new screening instrument for lower urinary tract dysfunction]. Actas Urol Esp. 2006;30(10):1017-1024.
doi pubmed - Corcos J, Beaulieu S, Donovan J, Naughton M, Gotoh M, Symptom Quality of Life Assesment Committee of the First International Consultation on I. Quality of life assessment in men and women with urinary incontinence. J Urol. 2002;168(3):896-905.
doi pubmed - Franic D, Franic Ivanisevic M, Verdenik I. Radiofrequency as the new opportunity in treating overactive bladder and urge urinary incontinence-a single-arm pilot study. Medicina (Kaunas). 2024;60(2):197.
doi pubmed - Jen E, Hsieh TH, Lu TC, Chen MC, Lee FJ, Lin CT, Chen SC, et al. Effects of pulsed-radiofrequency neuromodulation on the rat with overactive bladder. Neurourol Urodyn. 2017;36(7):1734-1741.
doi pubmed
This article is distributed under the terms of the Creative Commons Attribution Non-Commercial 4.0 International License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Clinical Gynecology and Obstetrics is published by Elmer Press Inc.